What Is Milialar? The Facts Behind This Fascinating Topic
Have you ever come across those small, white bumps on your skin, especially on your face? These tiny interlopers are referred to as milialar, and they’re actually quite prevalent. In this extensive guide, we’ll take a thorough plunge into the realm of milialar, revealing the enigmatic aspects of this captivating subject. What precisely are milialar? What leads to their occurrence? How can they be effectively treated? All of these inquiries and more will be addressed.”
Understanding Milialar: A Closer Look
What is Milialar?
Milia are minuscule, pearly-white protrusions that can manifest on the skin, occasionally being confused with pimples or acne due to their similar outward appearance. However, there are distinctive characteristics that differentiate them. Unlike acne, milia do not display any indicators of inflammation or redness. Typically ranging in size from 1 to 2 millimeters, these small protrusions can appear on different areas of the body. However, they are most commonly found on facial regions, especially near the eyes, nose, and cheeks.
The Intriguing Origins
The primary cause of migraine lies in the blockage of sweat ducts or oil glands beneath the skin’s surface. Sweat ducts and oil glands are responsible for regulating the skin’s moisture and oil levels. When these ducts or glands become obstructed, sweat, oil, or dead skin cells are trapped, leading to the formation of milia. Blocked sweat ducts are more common in newborns, whereas blocked oil glands are often seen in adults.
Milialar in Newborns
For newborns, the accumulation of dead skin cells, oil, or sweat during their time in the womb can result in the formation of milia. These tiny white bumps typically make their appearance a few weeks after birth and tend to resolve on their own within a few months. As the baby’s skin naturally exfoliates, the milia disappears.
Milia: Generally Harmless
“It’s crucial to highlight that milia are usually harmless and generally do not cause any pain or discomfort. ” Nevertheless, should you have any worries about your milia or if they are affecting your appearance in a negative way, it is strongly recommended that you consult with a dermatologist. They can provide a precise diagnosis and propose suitable treatment options tailored to your specific needs.
The Different Types of Milialar
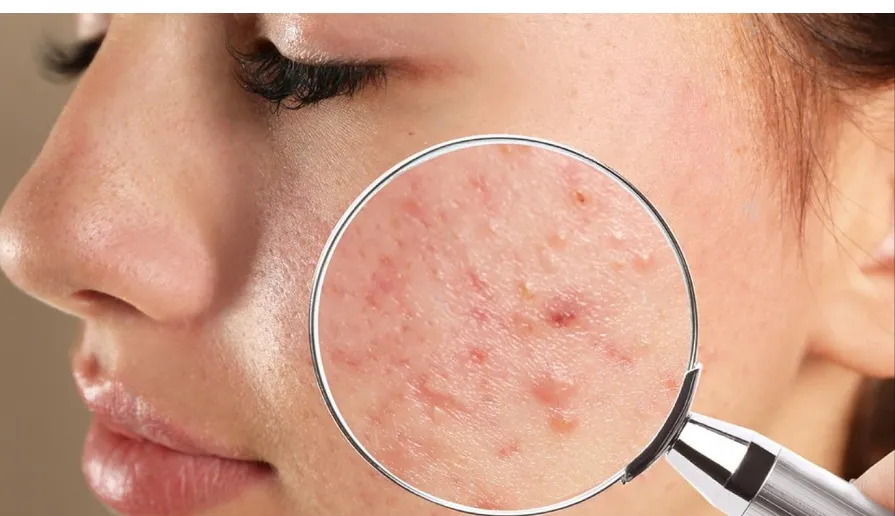
As we dive deeper into the world of migraine, it’s crucial to understand that this common skin condition comes in different forms. Recognizing the types of malaria not only helps in identifying them but also plays a role in finding the most effective treatment. Let’s explore the two main types of milia: primary milialar and secondary milialar.
Primary Milialar
Primary milia, also known as “milialar en plaque,” are small white or yellowish cysts that typically appear on the face, especially around the eyelids and cheeks. These milia develop when dead skin cells become trapped in the pores, causing them to harden and form cysts. Unlike acne, primary milia do not have inflammation or redness accompanying them, making them easily distinguishable.
Primary milia usually occur in infants and young children, but they can also manifest in adults, especially in areas exposed to prolonged sun exposure or skin trauma. Factors like repeated sunburns, the use of heavy cosmetics, or skin conditions like blistering disorders can contribute to the development of primary milia.
Secondary Milialar
Secondary milialar, as the name suggests, occurs as a result of an underlying skin condition or trauma. Unlike primary milia, secondary milia can develop in individuals of any age group and are often associated with damaged skin or disorders that disrupt the normal keratinization process.
Conditions like bullous pemphigoid, porphyria cutanea tarda, and genetic disorders such as Gardner syndrome can contribute to the formation of secondary milia.
Facial Milialar: A Common Concern
Our facial appearance is often regarded as one of our most significant attributes since it’s the initial aspect that catches people’s attention. Nevertheless, specific skin problems can detract from its allure and cause us to feel self-conscious.
One such issue is facial milia, which can be both frustrating and perplexing. In this section, we will demystify facial milia by exploring its causes and prevention, as well as the available treatment options.
Treatment Options
If you already have facial milia, don’t despair. Several treatment options are available to help get rid of these stubborn cysts:
-
Manual Extraction:
A dermatologist or esthetician can perform a procedure called manual extraction to remove the milia. They use a sterile needle or a small lancet to puncture the cyst and extract the keratin-filled contents carefully.
-
Chemical Peels:
Chemical peels can help exfoliate the outer layer of the skin, promoting cell turnover and unclogging the follicles. This can be an effective treatment for malaria.
-
Topical Retinoids:
Retinoids, such as retinol or prescription-strength tretinoin, can help speed up the cell turnover process and prevent the formation of new milia.
-
Cryotherapy:
Cryotherapy involves freezing the milialar with liquid nitrogen, causing the cyst to dry up and eventually fall off.
It’s essential to consult with a dermatologist or skincare professional to determine the most suitable treatment option for your specific case of facial milia.
Milialar On The Body: Common Locations and Potential Complications

Milia are small, white bumps that can appear on various parts of the body. While they are commonly associated with the face, they can also affect other areas. In this section, we will explore the common areas where milia can occur and the potential complications associated with them.
Common Areas Affected
Milia can crop up on different parts of the body aside from the face. Although they are more frequently found on facial skin, they can also appear in other areas with hair follicles. Here are some common locations where Milalar can be seen:
- Chest
- Neck
- Back
- Shoulders
- Arms
- Legs
The presence of milialar in these areas can be linked to the presence of hair follicles similar to those on the face. Hence, it’s crucial to be mindful of the possibility of their development in these regions too.
Potential Complications
While migraines are generally harmless and do not cause any discomfort, some potential complications may arise if they are left unaddressed:
-
Infection:
If the milia becomes irritated or scratched, the skin can become infected. It is important to avoid picking or attempting to remove milialar by yourself, as this can lead to skin damage and increase the risk of infection.
-
Scarring:
In some cases, milialar that have been tampered with or improperly removed can result in scarring. Therefore, it is crucial to seek professional advice for their safe removal.
-
Spreading:
While milia are not contagious, they can spread to adjacent areas if the underlying cause is not addressed or if proper skincare practices are not followed.
Being aware of these potential complications can help in taking the necessary precautions and seeking appropriate treatment for milia on the body.
Gentle Exfoliation
“Effective exfoliation plays a vital role in addressing milia and various other skin concerns. It involves the removal of dead skin cells and the unclogging of pores, which, in turn, reveal revitalized and refreshed skin. Nonetheless, it’s crucial to exercise caution when exfoliating in cases of milia to prevent exacerbating the condition. Here are some gentle exfoliation approaches worth considering:”
- Use a soft, damp washcloth to gently massage your skin in circular motions.
- Try a mild exfoliating scrub with natural ingredients like oatmeal or sugar.
- Opt for chemical exfoliants containing gentle acids like lactic acid or fruit enzymes.
Professional Treatments for Milia: Dermatologist-Recommended Procedures
When it comes to treating migraines and achieving a clear and healthy complexion, professional treatments are often the most effective solution. Dermatologist-recommended procedures, combined with topical medications and peels, offer a comprehensive approach to tackling this common skin issue.
Dermatologist-Recommended Procedures
Dermatologists are experts when it comes to skincare, and they can offer a range of treatments to help address many These procedures are specifically designed to target the underlying causes of milia and provide long-lasting results.
-
Extractions:
One popular dermatologist-recommended procedure is called extractions. During this treatment, a dermatologist uses sterile tools to extract the milia carefully.
- Microdermabrasion:
Another option is microdermabrasion, which involves gently exfoliating the skin to remove dead cells and unclog pores. This procedure not only helps with milia but can also improve overall skin texture and tone.
-
Electrocautery:
If milia are particularly stubborn or persistent, a dermatologist may suggest electrocautery. This procedure uses a small electric current to break down the milia and remove them.
Conclusion
In this journey through the intriguing world of Milalar, we’ve uncovered the secrets behind this common skin condition. From understanding its origins to exploring treatment options, we’ve provided a comprehensive guide to help you navigate the realm of milia.
Remember that morals, while perplexing, are generally harmless. Armed with the right knowledge and proper skincare practices, you can efficiently address and treat milia”If you ever have worries about your medical condition or need expert advice, don’t hesitate to reach out to a dermatologist. This way, when you come across those tiny, white bumps on your skin in the future, you’ll have the knowledge to effectively manage them in the realm of milia.
Also read more: Discover “Amazons GPT55X”: The Future of AI-Powered Technology
FAQs
1. What Is Milia, and What Causes It?
Milia are small, white bumps that commonly appear on the face. They occur when dead skin cells and keratin get trapped in the pores. Some skincare products, sun exposure, and skin damage can lead to milia, but the exact cause is unknown.
2. Can Milia be prevented?
In order to minimize the chances of developing milia, it’s crucial to follow a skincare regimen that emphasizes maintaining clean and exfoliated skin. Steer clear of heavy or oily skincare products, as they can block your pores. Safeguard your skin from sun damage by faithfully applying sunscreen daily and limiting prolonged sun exposure. If you already have milia, it’s advisable to refrain from trying to squeeze or remove them, as this may result in unwanted scarring.
3. Can Milia Be Treated at Home?
Milia can often be treated at home by gently exfoliating the skin and using products that promote cell turnover. Employ a mild facial scrub or a gentle chemical exfoliant to eliminate dead skin cells and ward off blocked pores. Nevertheless, if you are dealing with persistent or severe milia, it is advisable to seek guidance from a dermatologist to explore professional treatment alternatives.
4. Is milia contagious or harmful?
Certainly, malaria is non-contagious and does not present any health hazards. It is generally benign and tends to naturally resolve without the need for treatment. However, if milia are causing discomfort or self-esteem issues, you can seek professional help to have them removed.
5. What Should I Do If I Have Milia on My Body?
Aside from the face, milia can manifest in various other areas of the body. While they are typically benign, it’s crucial to refrain from causing irritation or scratching to prevent potential infections. If you happen to have milia on your body and require guidance on safe removal and preventive measures, dermatologists can provide you with expert assistance.

